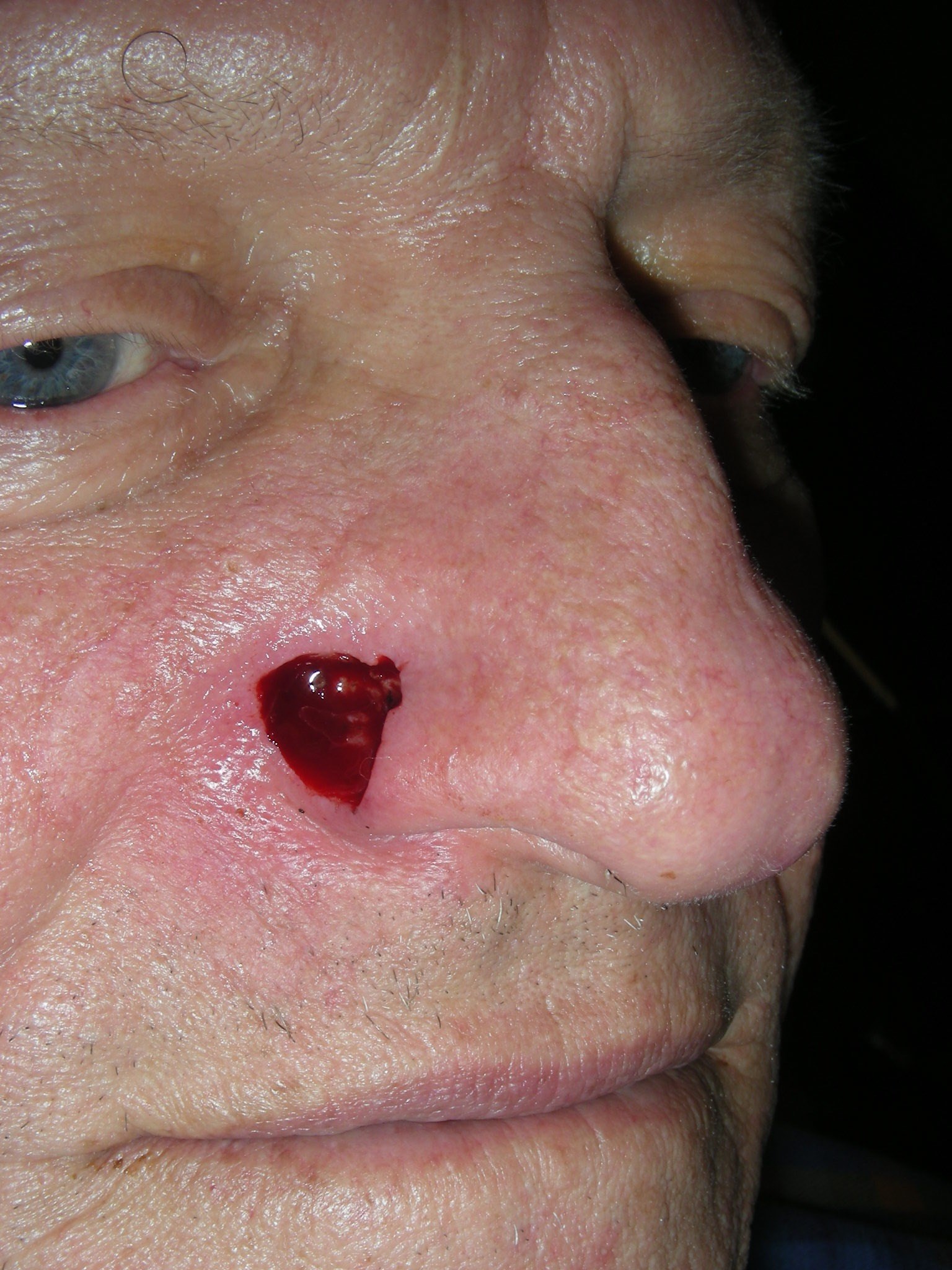
Mohs and Plastic Surgery for a Basal Cell Carcinoma on the Right Nostril
Patient
- Age:
- undisclosed
- Gender:
- Male
- Ethnicity:
- White
- Height:
- 5’ 6” - 6’ 0”
- Weight:
- 150 - 199 lbs
- Gallery:
- 38810
Procedure Details
Nasolabial Flaps
The are different variations of the nasolabial flap. Often plastic surgeons will perform a "pedicled nasolabial flap" designed as an "interpolation flap". This is the classic way that nasolabial flaps have been performed over the years. An area with skin redundancy or laxity is cut like a peninsula, lifted up and then bridged over normal skin to reach the cancer defect where the distant end of the peninsula is inserted and sutured to fill the cancer hole. However, in this patient we performed a different variation called a "nasolabial transposition flap". The transposition flap allows the skin to be shifted over into the defect without having a bridge of skin hanging over normal skin. When possible, avoidance of the skin bridge allows for easier healing, immediate aesthetic advantages, and much easier after-care. The skin bridges usually have raw undersurfaces that can bleed and ooze and make aftercare much more tedious. The skin bridge is also very unsightly for the few weeks it is in place. Last, skin bridges almost always require a second procedure weeks later to remove the skin bridge and “inset” the flap. Transposition flaps sometimes require a second procedure as well, but it is typically a much simpler procedure. Ultimately, we usually choose the procedure that will give the best long term result. But, in cases where the results should be similar either way, we lean toward transposition flaps instead of interpolation flaps.
Location
Popular Searches
*Right to Receive a Good Faith Estimate of Expected Charges. All information subject to change. Images may contain models. Individual results are not guaranteed and may vary.



&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)
&w=538&do-not-index)
&w=&do-not-index)